Audio
THR History and Development
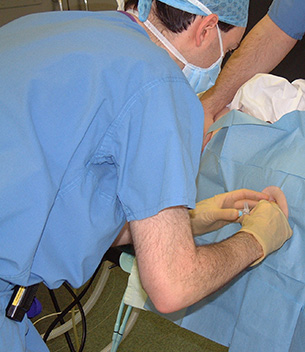
An anaesthetist performing a lumbar plexus block on a patient before hip replacement surgery.
Once the decision has been taken to perform a total hip replacement, it is not just a matter of turning up on the day and allowing everything to happen. What occurs pre-operatively, and immediately post-operatively, can be as important as the operation itself.
Pre-operative assessment
Many surgeons run pre-operative assessment clinics to assist in assessing the condition of the patient as a whole. There may also be an associated anaesthetic assessment clinic where more severe non-surgical problems are considered. The kinds of checks included in a preoperative assessment vary, but some of the commonest are as follows:
- Haemoglobin level (blood count)
- Blood cross-matching
- Electrocardiogram (ECG/EKG)
- Urea and electrolyte estimation
- Urine testing
- X-Rays (chest and hip)
Thought should also be given pre-operatively about what is going to happen post-operatively. What facilities does the patient have at home? Will family and friends rally round in support or is it necessary to book a convalescent home? What kitchen and bathroom aids exist at home, if any? Is there a steep, winding staircase leading to the bedroom, implying that the patient's bed should be brought downstairs for a few weeks once they have returned home? There are many questions to be asked before hip replacement surgery. Don't wait until you arrive in hospital to ask them!
Admission to hospital is normally either the day before surgery or on the day of the operation itself. The attraction of coming in on the day of surgery is that it allows a patient to remain in the familiar surroundings of their home right up to the last minute.
The operation
In most modern operating theatres in the United Kingdom, anaesthetics (general or local) are administered in an anaesthetic room immediately adjacent to the operating theatre. However, this situation does not always apply worldwide. In some countries and in some hospitals, the anaesthetic is administered in the operating theatre itself.
Assuming that a general anaesthetic has been chosen (hip replacements can also be performed under local anaesthesia), the process of putting a patient to sleep is called induction. For this, only a small needle need be used. Once the patient is safely asleep, the anaesthetist will then be able to pass a breathing tube (endotracheal tube) to control breathing throughout the operation. Sometimes, once the patient is asleep, a local anaesthetic injection can be given to supplement the general anaesthetic. This can be an epidural injection, perhaps a spinal injection, or what is called a regional nerve block. This latter form of anaesthesia is quite widely undertaken as it does not paralyse the whole lower limb but selectively anaesthetises specific nerves in order to relieve pain after surgery but not necessarily to prevent movement.
Once asleep, the patient is wheeled by trolley into the operating theatre, lifted onto the operating table, and positioned accordingly. In the author’s practice the patient is positioned on their side, but in some practices the patient may be supine throughout the operation. The surgical team then scrubs up, dons their gowns and surgery commences. Before any surgical instrument is used, however, it is essential that the patient's skin is cleaned. A special solution is used to kill all skin bacteria. However clean we think we are, it is a sad fact that the normal human skin surface is crawling with little beasts. It is vital they are killed before surgery begins otherwise there is an increased risk of the hip replacement becoming infected. This process is called skin preparation ( or ‘prepping’) and is followed by the application of surgical drapes. Once the drapes are in position the operation proper begins.
Many people are involved with a hip replacement. As well as the surgeon performing the operation, there may also be a surgical assistant standing opposite him. Occasionally there can be two assistants, and sometimes three! An assistant’s job is to help with tasks such as patient positioning, tissue retraction, blood vessel coagulation, stitch cutting, and the like. A theatre sister hands the instruments to the surgeons - a good sister will not even need to be asked what instrument is required next. She (or he) will be so experienced that the operation will be second nature. Helping the theatre sister is a circulating nurse (sometimes called a ‘runner’) and helping the anaesthetist will be an operating department practitioner (ODP). Added to these individuals will be recovery nurses, instrument cleaners, auxiliaries, and administrators. At the last count a primary hip replacement required fourteen separate individuals within the theatre complex alone, few of whom the patient ever sees, or is aware of.
A typical operating time would be approximately 90 minutes from first incision to final skin closure (skin-to-skin time in the trade). However, because of anaesthetic and recovery, the time away from the ward may be much greater (as much as three hours, or more). For relatives waiting for news this can be a worry, so be prepared for a long absence of your loved one before information is available. It does not mean anything is going wrong! Full operative details will not be given here, although can be found in Richard Villar’s Understanding Hip & Knee Arthritis Surgery.
After the operation
Once the final skin stitch, or staple, is inserted, the patient is transferred from the operating table to their bed. It is usual at this stage for the leg to be held in some form of immobilising device. The simplest and most widely used of these in an abduction pillow. This is a triangular pillow that is placed between the patient's legs to hold them apart. This abducted position is the most stable position a hip can adopt.
Mobilisation normally begins on the first or second post-operative day. Surgical drains are generally removed after 24 hours, although in some cases may remain in place until 48 hours. Blood tests may also be undertaken 24-48 hours after surgery while prophylactic treatment may be given to reduce the chances of thrombosis forming in the calf veins. This can take the form of stockings, anticoagulants, or even simple aspirin. There are many different ways of tackling the thrombosis issue. Antibiotics may also be given, although are normally provided in a few high intravenous doses to cover the period immediately surrounding surgery.
While mobilisation takes place it is usual for the patient to be continually instructed in the permitted and forbidden activities after total hip replacement. The aim of this is to reduce the chance of a post-operative dislocation. For example, one would normally not wish a patient to bend the hip to more than 90 degrees for a period after surgery, or to cross their legs, or to bend down too low in order to tie a pair of shoe laces. As time passes, so these rules can often be relaxed slightly, but in the early days after total hip replacement it pays to be very careful with hip positioning. The amount of pressure that is allowed to be placed through the operated leg also varies from patient to patient and surgeon to surgeon. However, it is normal for some form of walking support to be used for between four and six weeks after surgery. Initially this support may be in the form of a walking frame but the patient will generally move on quite rapidly to using a pair of crutches and from there to one or two walking sticks. Most patients will be discharged home using two crutches for walking support.
The time for discharge is very variable, although there is a trend for the hospitalisation period to be reduced quite significantly these days. In the mid-1990s it was quite normal for patients to stay in bed for at least two days after surgery before beginning their mobilisation and to stay in hospital for 10-14 days. Now, many patients are discharged home by the third or fourth post-operative day, seemingly without any greater chance of complications. Mobilisation, in some units, can begin within a few hours of surgery being completed.
