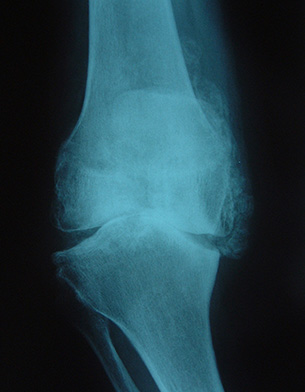
X-Ray of a patient with severe osteoarthritis (OA) of the knee. Most of the articular cartilage (gristle) has been worn away and the joint is very deformed. This would be a typical reason for offering a total knee replacement.
If a joint replacement needs to be redone, for whatever reason, it is called revision surgery. Generally, this is big surgery, more demanding, more time-consuming, and more complicated. There is need for highly specialist surgical techniques and equipment.
Sometimes it is necessary for revision surgery to be performed in two stages, a two-stage revision. This is most often employed for infected knee replacements. The first stage involves the removal of the infected components. A period then follows where no replacement is left in the knee at all, although sometimes the surgeon will leave an antibiotic spacer in position. Once the infection has settled, so it is possible to undertake the second stage, where knee components are reinserted. Occasionally, even a two-stage revision is insufficient to settle an infection, in which case a three-stage or even four-stage operation may be required.
With a revision operation the surgeon may be faced with weak bone, often seen when a knee replacement has been in place for a long period. This weak bone may need to be buttressed with bone graft. If bone graft is used, this may be obtained from either another location in the patient, or even a bone donor. The use of donated bone is called allografting.
Sometimes a revision operation is not possible. Should this be the case, a number of choices exist. The surgeon can attempt to fuse the knee (arthrodesis), or can simply remove the components and leave the joint as it is (excision arthroplasty). This latter operation leaves behind a rather weak, floppy knee, but this may be better than the final solution for remedying a failed knee replacement - amputation.
